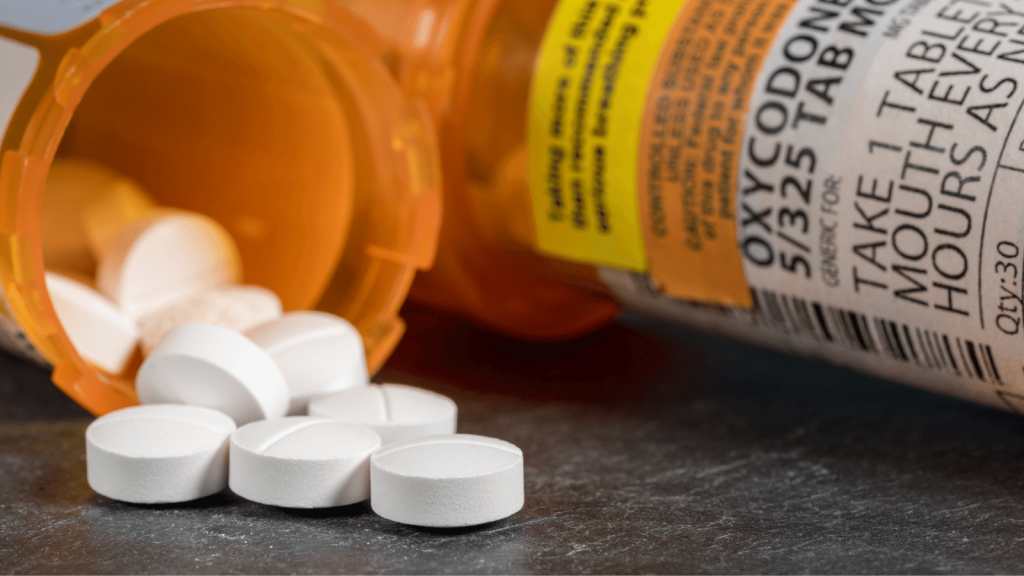
In Canada, the ongoing public health crisis of opioid overdose and deaths is worsening. Between January 2016 and June 2021, 24,626 persons died in Canada because of opioid overdoses, with latest figures indicating a frightening increase of 19 deaths per day. With a 66 % increase in death year over year, the COVID-19 pandemic in Canada has exacerbated the opioid problem, and we are still learning about the causes and risks that contribute to these terrible overdoses, which involve both prescribed and non-prescribed opioid use.
Why is there an increase in opioid-related harms?
The following reasons may have led to the rise in opioid-related harms:
• Social isolation and pandemic-related stress1
• Erratic unregulated drug supply due to border and travel restrictions1
• Restricted accessibility of healthcare services1
The pandemic has affected virtually all services and therapies accessible to people suffering from chronic pain, addiction, and mental illness.
Anxiety alone is a huge cause for drug use, and what could be more stressful than the current pandemic? People who formerly used drugs with a friend are now doing so alone, with no one to contact 911 or administer naloxone. COVID-19 overburdened emergency rooms and hospitals, and they may not have had the time or resources to address addiction.
Opioids are undeniably effective in the treatment of certain types of pain, such as post-operative, palliative, and cancer pain. However, the fact that around 10% of those who are prescribed opioids go on to develop an opioid use disorder (OUD) is cause for concern2. Furthermore, problematic opioid usage isn’t just an individual issue; it’s also a ‘proximity’ issue for friends, family, and communities.
Who are most likely affected by the opioid crisis?
The opioid issue affects some communities and populations disproportionately, such as males aged 20 to 49 who work in the construction industry3. Chronic pain is a major issue in the trades and construction industry, with 32% of workers over-indexing for chronic back pain alone. Construction workers are estimated to account for 30% of all opioid-related deaths. Additionally, workers with a substance use disorder (SUD) miss an average of 14.8 days per year, while workers with OUD miss an average of 29 days per year4. This points to a rise in the number of construction workers seeking treatment for chronic pain and OUD.

Chronic pain, however, is rarely isolated; it is frequently linked with sleep disturbances and emotional distress, forming the well-known “Pain Triad.” Opioids are currently the most used drug to treat the Pain Triad. Because no single medication can target all three arms of the pain triad, prescribers frequently turn to multiple high-risk drugs, including opioids, that together increase the abuse potential and worsen symptoms.
As a result, there has been a lot of interest in potential alternatives.
The opioid overdose crisis is worsening during the COVID-19 pandemic with many communities across Canada reporting record numbers of opioid-related deaths, emergency calls and hospitalizations. We can all play a role in supporting those who use substances.
If you or someone you care about is in need of assistance – Get help now.