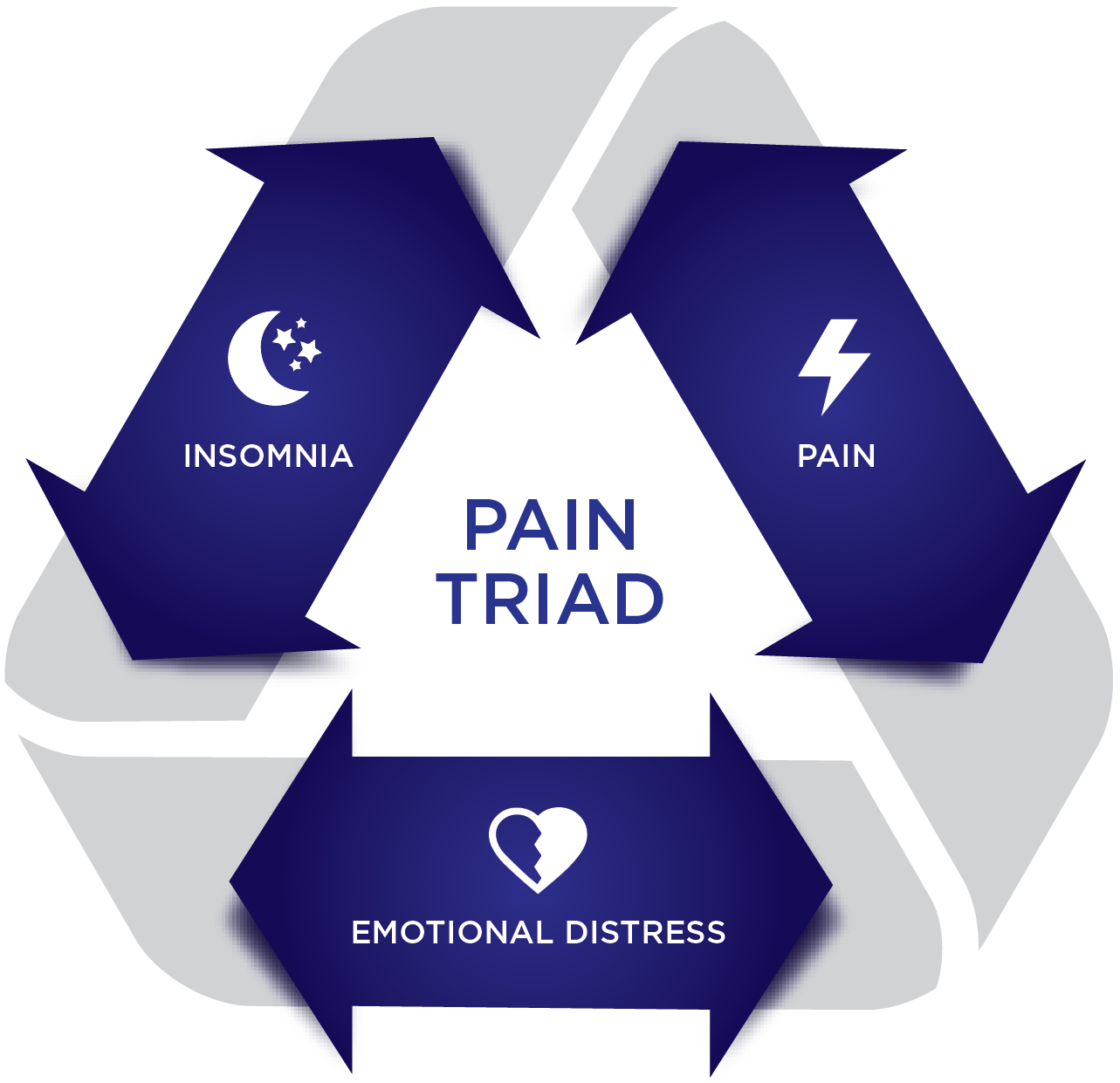
Chronic pain is rarely isolated; it is frequently linked with sleep disturbances and emotional distress, forming the well-known “Pain Triad”. These three interconnected ailments can affect a person’s quality of life. For example, a high level of pain can lower your mood and reduce your quality of sleep.
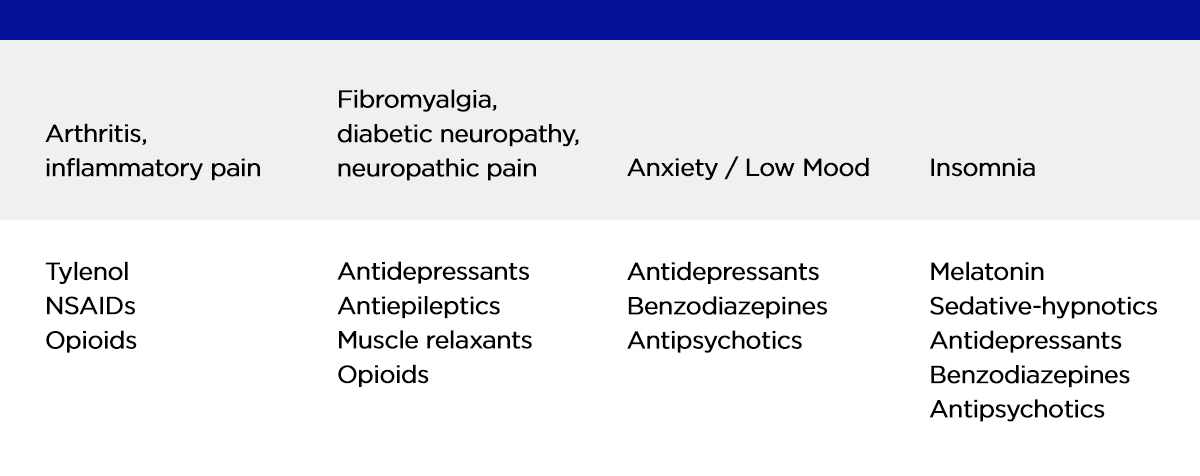
Medications typically used to treat the Pain Triad
The drug classes that correlate to the three pillars of the pain triangle are listed below1. Medical cannabis is a promising alternative for all, and it is likely to avoid the negative side effects associated with these drugs, particularly opioids.
Medical cannabis as an alternative solution to the opioid crisis
Medical cannabis is a promising alternative to opioids for the treatment of chronic non-cancer pain2, which is the most common indication for its use. Other areas where cannabis has showed promise to date are in fact covered by drug classes overwhelmingly used to the three pillars of the pain triad. Moreover, cannabis may well spare patients many of the side effects associated with opioid use3.
For those interested in using medical cannabis as an adjunct therapy option to opioid, Starseed offers several product options that maybe helpful for patients. Starseed’s clinic partner ‘North Star Wellness’ is also available for medical cannabis consultations free of charge. With 9 clinics across Ontario and a team of expert health care professionals, North Star Wellness offers in-person and telemedicine consultations for patients in need of education and medical authorization for cannabis.
Register and book your appointment today.
References:
[1] National Pain Centre (2017). The 2017 Canadian Guideline for Opioids for Chronic Non-Cancer Pain. Hamilton, ON: McMaster University. Retrieved from http://nationalpaincentre.mcmaster.ca/documents/Opioid%20GL%20for%20CMAJ_01may2017.pdf
[2] Benedict, G., Sabbagh, A., & Conermann. (2022). Medical cannabis used as an alternative treatment for chronic pain demonstrates reduction in chronic opioid use – a prospective study. Pain Physician Journal, 25, E113-E119. Retrieved from https://www.painphysicianjournal.com/current/pdf?article=NzQwOA%3D%3D.
[3] Ergisi, M., Erridge, S., Harris, M., Kawka, M., Nimalan, D., et al. (2022). An updated analysis of clinical outcome measures across patients from the UK medical cannabis registry. Cannabis and Cannabinoid Research, X(X), 1-10. Retrieved from https://www.liebertpub.com/doi/epdf/10.1089/can.2021.0145.